Remote monitoring leads to earlier detection of infections, enabling treatment in the community, avoiding re-admission to hospital
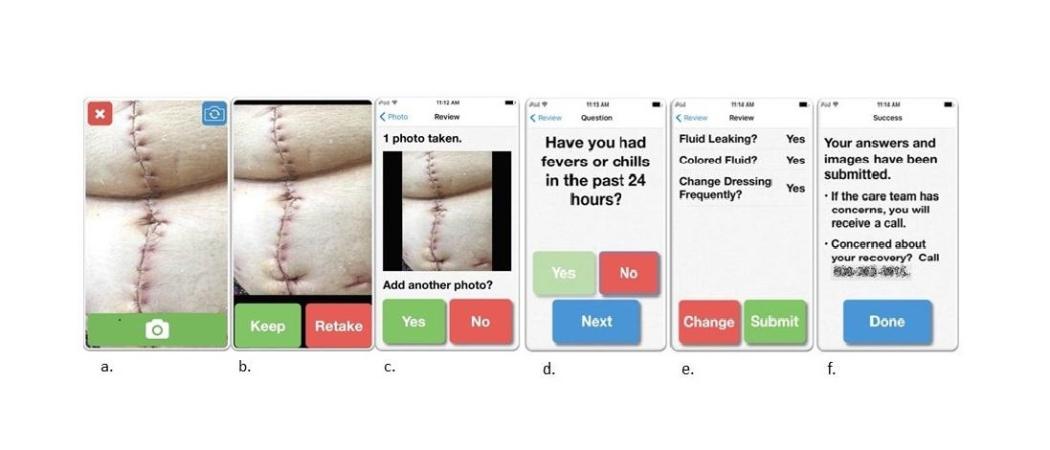
A new smartphone app, WoundCare, is enabling patients to remotely send images of their surgical wounds for monitoring by nurses, allowing earlier detection of surgical site infections (SSIs) and prevention of hospital re-admissions.
SSIs are the most common hospital-acquired infection and the leading cause of hospital re-admission following an operation.
Given the prevalence off SSIs, researchers at the Wisconsin Institute of Surgical Outcomes Research, Department of Surgery at the University of Wisconsin, Madison, set out to assess if postoperative wounds could be effectively monitored by having patients upload photos through the WoundCare app and answering a few brief questions to gather information not easily captured through images.
Patients cannot identify infections and frequently ignore or fail to recognise the early signs of wound complications, according to a report of the research published in the Journal of the American College of Surgeons.
This leads to the “common and frustrating scenario” where patients present to a routine, scheduled clinic appointment with an advanced wound complication that requires readmission, and which may require another operation. It is likely infections would be amenable to outpatient management if detected earlier.
The study enrolled 40 vascular surgery patients. There was an overall data submission rate of 90.2 per cent among participants, and submissions were reviewed within an average of 9.7 hours.
During the study, seven wound complications were detected, and there was one false negative.
“We set out to come up with a protocol where patients could become active participants in their care and allow us to be in closer communication and monitor their wounds after they leave the hospital,” said lead study author and general surgery resident, Rebecca Gunter.
“This approach allows us to intervene at an earlier time, rather than waiting for patients to come back in after the problem has already developed past the point of being able to manage it on an outpatient basis.”
Patients were enthusiastic about ease of using the app and the reassurance they felt having their wounds regularly monitored. The nurse practitioners responsible for reviewing the images confirmed the value of the photos and noted a positive impact on patient satisfaction.
However, nurses also said it is difficult to find time to review the wound images on top of an already heavy clinical workload.
The study authors say the success and sustainability of a post-discharge wound monitoring protocol calls for a dedicated transitional care programme - and not simply adding a task to the current staff workload.
In addition to the patient safety and satisfaction aspects, the protocol has a cost savings component. SSIs are the most expensive hospital-acquired infection, costing an average of nearly $30,000 per wound-related re-admission, and an estimated $3 -$10 billion annually in the US.
“If you could imagine saving the cost from the number of patients whose re-admission you were able to prevent, that result could provide significant savings to the health system,” Gunter said.
Quantifying cost-savings was not part of the research but is an important area of focus for future studies.
One limitation of telemedicine protocols using smartphones is that not every patient has the necessary technology or knowledge to upload images. The Wisconsin research team addressed this issue by giving participants training in how to use the WoundCheck app.
Each patient was given an iPhone 5S and an accompanying visual reference guide to further assist in using the phone and app.
Gunter said this approach was very successful in giving patients knowledge and access to technology so they could participate in the study. The model is easily adaptable to other medical centres, whether through providing participants with a phone, having a rotating supply of phones at hospitals for patients to borrow, or relying on a patient’s own device.
“We have demonstrated that a population of complex and high-risk patients, many of whom are older adults and novice smartphone users, can complete this protocol with high fidelity and satisfaction,” the research concludes.
Reference: Feasibility of an Image-Based Mobile Health Protocol for Postoperative Wound Monitoring.




 A unique international forum for public research organisations and companies to connect their external engagement with strategic interests around their R&D system.
A unique international forum for public research organisations and companies to connect their external engagement with strategic interests around their R&D system.