More prevention, improved primary care and an integrated, patient-centred approach is the route to making health systems resilient. Underpinning all this will be better data, says report on State of Health in the EU
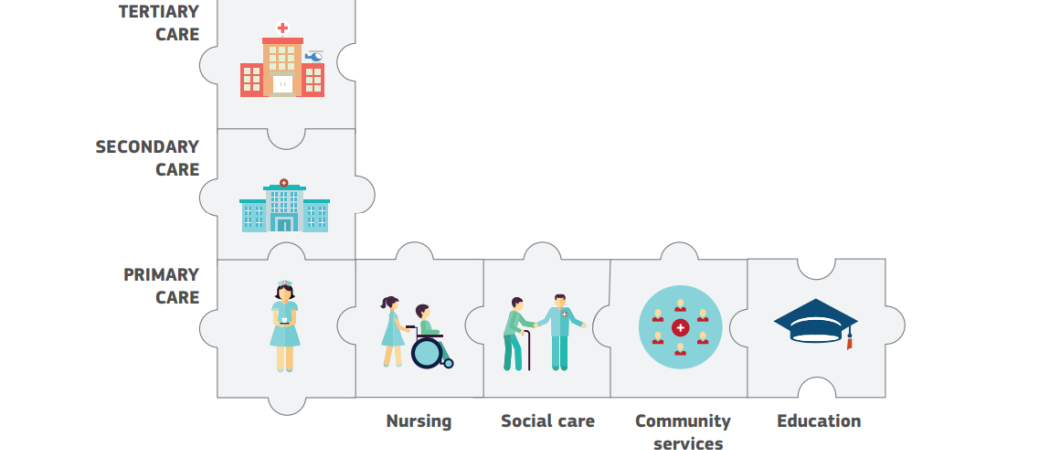
Key elements in designing a successful integrated care system
The Commission has called on member states to rethink how they run their health systems, setting out five policy levers it says will help to ensure they are fit-for-purpose and provide patient-centred care.
The recommendations are made on the back of 28 in-depth country profiles published last week, which highlight a disparity in investment and performance across Europe - and point to how rising demand is straining even the best resourced systems.
“By offering comprehensive data and insights, we aim to support national health authorities in tackling the challenges and in making the right policy and investment choices. I hope they will make good use of it,” said Vytenis Andriukaitis, Commissioner for Health.
Policy lever number one is prevention, which despite being the key to avoiding ill health, attracts only 3 per cent on average of health care budgets. That is coupled with limited political attention and minimal stakeholder engagement, according to the Commission’s diagnosis the state of health in the EU, compiled with the assistance of OECD and WHO.
“Spending only 3 per cent of our health budgets on prevention, compared with 80 per cent on the treatment of diseases, is simply not enough” Andriukaitis said. “We need to enshrine health promotion and disease prevention into all policy sectors to improve people’s health and reduce pressure on health systems.”
Health promotion and disease prevention pave the way for more effective and efficient health systems. It is also a means to tackle the social inequalities of health across Europe that are illustrated, amongst other factors, by differences in cancer screening or physical activity between people with higher and lower incomes and education.
Breaking the “vicious cycle” of ill health and poverty will require collaboration with other policy fields, the Commission says. “There is now a need to bring together lessons learned and good practices, in order to transpose, pilot and up-scale them in other countries, contexts and settings,” according to companion report to the 28 country profiles.
The country profiles show significant disparities between population groups within most, if not all member states. These follow a clear social gradient, reflecting the circumstances in which people live, their jobs and their lifestyles.
Poverty, unemployment and material deprivation are all major risk factors for mental and physical health. They contribute to poorer health and to an earlier onset and a higher number of chronic conditions. Recent research even points to low socioeconomic status as the third most important factor associated with increased mortality, after smoking and physical inactivity, according to the companion report.
Strengthening primary care
In addition to better health promotion and prevention, strong primary care plays an important role in reducing health inequalities.
Effective primary care also increases the quality of healthcare overall, making systems more patient-centered and resilient.
At the same time, the budgetary constraints member states are facing call for a changing role for hospitals, with shorter stays and a reduction in the number of unnecessary treatments.
Better primary care is the way to achieve this. Amongst other factors, primary care guides patients through the health system and helps avoid wasteful spending, coordinating care so patients are given the most appropriate services in the right setting, and reducing avoidable hospital admissions.
“We need better access to primary care so that the emergency room isn’t people’s first port of call,” Andriukaitis said.
Strong primary care is also a powerful means of involving patients in decisions about their healthcare and encouraging them to actively participate in the care process. The evidence suggests that investment in patient-centred communication substantially increases the number who adhere to the recommended course of treatment.
The report points to innovations that are enabling primary care to provide a wider range of treatments and take care of conditions that were previously addressed only by specialised care or in hospital settings.
These include tailored diagnostic devices, such as miniaturised ultrasound scanners and portable pulmonary function tests that can preclude hospitalisation and reduce waiting times for patients. Home-based devices, such as a 24-hour electrocardiogram enable patients to significantly reduce the time they spend within health care facilities.
The consequences of inadequate primary care
The right combination of incentives can help systems achieve optimal delivery not only of primary care, but also of secondary care, hospital, and emergency services. Given this, building in a gatekeeping or referral system is increasingly part of the mix. However, more than one in four patients across the EU still visits an emergency department because of inadequate primary care.
The EU Expert Group on Health Systems Performance Assessment is currently working on identifying tools and methodologies for assessing the performance of primary care systems, and it is expected to present its findings in the first quarter of 2018.
The rising burden of chronic disease and multi-morbidity requires member states to confront the current fragmentation and move towards integrated health systems that link or coordinate providers along the continuum of care, with the patient at the centre.
Here, a key challenge is to overcome the fragmentation of services and medical records, since patients with complex conditions increasingly need experts from different specialities, require services from a number of different carers and institutions and to access care in more than one place in the system.
The challenge for many countries is to develop care delivery systems that bring together professionals and skills from different areas, within and outside the health system.
While to date there has been little progress towards integrated models, the initial evidence indicates this approach improves effectiveness, accessibility and resilience, according to the Commission’s report.
The need to reform and move to integrated healthcare also underlines the importance of having the right skills mix and training, and of being able to share information effectively.
That brings the Commission to the next policy requirement, which is that member states put in place proactive health workforce planning and forecasting to make health systems resilient to future shocks.
Health systems need to apply new technologies, products and organisational change, all of which depend on having a workforce of sufficient capacity and with the right skills and flexibility.
This is a demanding requirement: Europe’s 18.6 million health and care workers represent 8.5 per cent of the EU’s total workforce. They are involved in a wide range of activities, promoting healthy lifestyles, preventing, diagnosing and treating ill-health.
The number of workers in the sector grew by 13 per cent between 2008 and 2016, a net creation of 2.1 million jobs. That represents the largest absolute increase of any economic sector during this period. According to an analysis by the European Centre for the Development of Vocational Training, this trend is expected to continue, with the creation of about 1.8 million additional jobs between 2015 and 2025, an increase of 7.8 per cent.
Despite the huge number of health care workers, many countries are confronted with critical workforce problems, including supply and distribution of skills, and an out of date skills mix. The Commission says reforms in initial education and training programmes, and investment in continuous professional development, are needed to foster new and appropriate skill sets.
Data is the lynchpin of policy
If the patient is to be at the centre, member states need better data. Health systems need to provide the right services to the right people at the right time. Given this, policy makers need to know more about their current and future patients, and to have robust health data as an input to evidence-based policy.
Reliable and policy relevant health statistics are required to inform health promotion and disease prevention, to improve primary care, support integration across the system, and to aid better workforce planning and forecasting.
But as a number of the member state profiles show, policy makers are facing major knowledge gaps. This is constraining efforts to improve the effectiveness, accessibility and resilience of health systems.
Data on patient experiences and outcomes are needed to inform policy making across the spectrum. This will provide the information and tools to more effectively treat patients with increasingly complex conditions and multiple morbidities, and to deliver the outcomes that patients value most.
Whether this is survey data or real-world data, a precondition is a coherent data governance framework, with clear rules about ethics and confidentiality. In the next few years, the Commission will support the OECD in the rollout of its first Patient-Reported Indicators Survey (PaRIS).
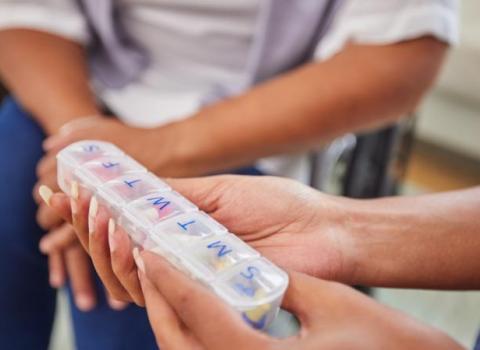
PaRIS will focus on patient-reported outcomes, such as whether a treatment reduced pain or enabled a person to live more independently.
In addition, the international survey will cover experiences reported by patients more broadly, asking them whether they felt involved in decisions about their care, or whether a treatment was appropriately explained to them.
While these data exist in some regions or countries, this will be the first large-scale attempt at a reliable comparison across countries and is expected to fundamentally improve the tools available for health policy and practice.
Country profiles:
https://ec.europa.eu/health/state/country_profiles_en
Companion Report:
https://ec.europa.eu/health/state/companion_report_en
OECD PaRIS survey:




 A unique international forum for public research organisations and companies to connect their external engagement with strategic interests around their R&D system.
A unique international forum for public research organisations and companies to connect their external engagement with strategic interests around their R&D system.